Post-traumatic stress disorder can have far-reaching effects on an individual’s life, making even the simplest tasks an ordeal. Noreen Tehrani finds out how employers can help workers who are suffering.
When people are exposed to the horror of death, serious injury or sexual abuse, normal coping mechanisms may become overwhelmed, causing the brain to respond in a way that is designed to protect their life. This immediate adaptive response to trauma can include an increased vigilance or alertness to other potential dangers, a tendency to avoid similar dangerous situations and flashbacks to the event in the form of images, thoughts and dreams.
At the time of the traumatic exposure, individuals may also find themselves operating on “auto pilot” when dealing with the situation, devoid of strong emotions that may prevent them from taking the appropriate defensive actions. If human beings had not developed these automatic responses to trauma, it is unlikely that we would have survived as a species. After exposure to even the most traumatic event, most people return to normal functioning within a month or so – and while they may have unpleasant memories, the majority are able to get on with their lives.
However, for a small number of people the return to normality does not occur. Instead, they get stuck in a state of continually seeking to avoid reminders of the event, become sensitive to anything related to the traumatic exposure and re-experience the traumatic event in dreams and flashbacks. When this happens, the individual can find it impossible to return to normal functioning. It is at this time that people may be diagnosed as suffering from post-traumatic stress disorder (PTSD). While initial reactions to extreme danger and horror allow people to adapt and come to terms with the event, longer-term trauma symptoms do not allow either. The presence of PTSD is regarded as a failure of recovery rather than an expected outcome of a traumatic exposure.
In a recent review of the clinical definition of PTSD, the criterion for traumatic exposure was widened to include secondary traumatic exposures (for example, body recovery or dealing with child abuse materials) (Tehrani, 2011). The review also added a fourth cluster of symptom-related changes in thinking and mood; symptoms include memory loss, a sense of detachment, ruminating on the traumatic event, loss of interest in the future and persistent negative self-beliefs. This fourth symptom cluster combines responses that would have had value during the trauma – such as dissociation, which reduces the physical and emotional pain of the trauma – with symptoms that are secondary responses to being traumatised, such as the individual believing that they have no future and that no one can be trusted.
Causes of personal and workplace trauma
Some events have the power to overwhelm the brain’s coping processes and lead to an increased incidence of PTSD. Among the most “toxic” events are: being under fire in an armed conflict; being raped or otherwise sexually assaulted; involvement in a transport crash/collision; witnessing the sudden death of a close family member or friend; being physically attacked; exposure to a major disaster; and fearing for your life and physical safety (see box 1, below). People can become traumatised through direct exposure, witnessing another person suffering a trauma, hearing of a traumatic event happening to a close family member or friend, or being an emergency responder.
In studies that have surveyed large populations, it has been found that up to 92% of men and 87% of women will experience at least one traumatic event in their lifetime. This rate of traumatisation is greater for people who come from violent urban areas or from parts of the world where terrorism or other forms of conflict are common.
Box 1: Common sources of traumatic exposure |
||
|
|
|
While organisations may not be responsible for the personal traumas of their workers, the fallout from these traumatic experiences will affect employees’ attendance and their ability to work. Understanding the effects of trauma and how it can be handled in the workplace is therefore an important skill, given that most workers will have or have had experience of a traumatic event.
The workplace can also involve traumatic exposures; here, the organisation has a legal duty of care towards its workers and a responsibility to do something to reduce the risk of harm. Almost anyone could witness a colleague having a heart attack, stroke or suffering a serious injury at work. This can be extremely upsetting, particularly if the person involved dies in the workplace. The employees of some organisations are exposed to a much higher possibility of trauma than the norm, and therefore these organisations have a greater duty to undertake role risk assessments to identify those most at risk and to work to reduce the risk or treat it where it cannot be removed.
There are several types of role where workers are most likely to encounter traumatic exposure, including where employees are:
- working with machinery, vehicles, chemicals or in construction, where there is a potential danger of physical injury or death;
- enforcing the law or regulations, where the officer or worker is liable to violence or threats of violence;
- providing services to members of the public where there may be exposures to violence, threats or physical injuries and diseases;
- being exposed to graphic traumatic materials or artefacts.
The direct effect of physical injury and death is well recognised, but many organisations fail to acknowledge the effect of a traumatic death on first aiders and other rescuers, colleagues and bystanders. There are examples where the body of someone who died or was killed at work is not covered, which exposes colleagues and friends to unnecessary distress.
Many employees are involved in law enforcement work. Stopping someone from doing something that they want to do is never easy and there is often resistance, which can range from police officers dealing with terrorism, to social workers removing children, to prison officers imposing cell searches, to teachers requiring students to behave with respect, to traffic wardens issuing parking tickets and to immigration officers refusing permission to stay. Any of these – among many other roles – can create conflict that can lead to violence or threats of violence
Because people pay local and national taxes, many hold the belief that they have an entitlement to a particular standard of service, and often these expectations are unrealistic. Nevertheless, when expected services are not made available there can be a reaction against a public servant who is perceived to have withheld access.
Violence is not uncommon in A&E departments, where waiting times may be extended because of the volume of work. Threats may be made against planners and architects who make decisions that affect the life or amenities of a community, and professionals may be vilified and threatened on the internet when they make a controversial decision. All of these situations can be traumatic for the people involved.
Secondary trauma is a new concept, but one that is important to consider. Many people who work with people in the community become exposed to traumatic images, testimony and other materials. Lawyers read in detail the sexual abuse of children in order to defend them, probation officers work with perpetrators of distressing crimes, social workers handle cases of extreme abuse and the police investigate traumatic crimes. All these groups of workers are vulnerable to secondary trauma.
How can organisations help?
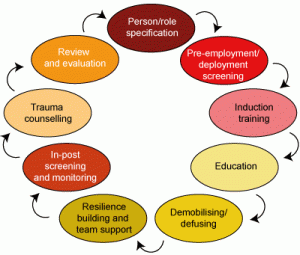
It is essential that companies identify which of their workers are most at risk of a traumatic exposure and employ a process for managing the risk and treating the outcomes when the risk could not be eliminated. The risk management approach (see image below) has nine elements that are designed to ensure the safe operation of the organisation. The stages are: person specification; pre-employment/pre-deployment screening; induction training; education; demobilising/defusing; resilience building and team support, in-post screening and monitoring, trauma counselling, and review and evaluation. While not all stages may be relevant to all situations, the following brief descriptions will help organisations decide on an appropriate level of support for their workers.
The risk management approach |
 |
Person specification and role risk assessment
It is important to understand the nature of each role and to create a person specification. There are two elements to any role: the technical skills required to undertake the work; and the personal skills that enable the person to carry out their role without undue stress. The role specification provides the information required to undertake a role risk assessment in which all the role-related risks can be identified and evaluated.
Pre-employment screening
For the roles identified as involving high levels of exposure to trauma, pre-employment screening is essential to identify people with the psychological resilience who are suitable to undertake a role safely. Research on pre-employment screening has identified a number of psychological questionnaires that are particularly good at identifying candidates who are resilient and suited to this work (Tehrani, 2011). Most of the questionnaires require the administrator and interpreter to have undergone training in psychometrics.
Induction training
When someone new joins an organisation where they may be exposed to trauma, it is important to have a comprehensive induction programme.
Resilience is dependent upon personal characteristics, the level of support available to the individual and their coping style. In order to build resilience, the induction process should involve an understanding of the dangers involved in the work. The length of time individual workers need to build their personal resilience can vary, but it would be unlikely that the induction process would be less than one month or longer than three months.
During the induction process there should be regular reviews and consolidation sessions where the member of staff should be encouraged to discuss and consolidate their learning.
Education
The education programme should be tailored to the needs of workers, supervisors and managers, and should provide simple information on the nature of trauma, secondary trauma and burnout. There should be descriptions of the common symptoms and suggestions of ways to reduce distress by simple lifestyle activities and coping strategies. Reference needs to be given to the individual and organisational responsibilities to protect health and wellbeing.
Demobilising/defusing
These two processes are normally carried out by the leader of the team or unit following a particularly difficult or distressing incident.
Demobilising involves the team leader getting the team together to thank everyone for their efforts, recognise what has occurred, provide information on any action that has been taken and give information on the possible effect the incident may have on workers and how this can be reduced.
Defusing is used when a team member is particularly affected by an incident and involves the leader providing support and identifying whether or not further support is required.
Resilience building and peer support
Where there are teams of workers undertaking similar tasks, it can be helpful to set up resilience-building sessions that allow team members to discuss issues or difficulties that arise within their work and to encourage other members of the team to work with them to identify solutions.
While this kind of conversation often occurs naturally, specifically setting aside time for people to get together for this purpose can provide opportunities for the team to learn from each other and reduce the barriers to open discussions on the effect of the work.
In-post screening and monitoring
Having undertaken pre-employment screening, it is important to then monitor workers. This should be done using the same tools that were used in the pre-employment screening, looking for evidence of anxiety, depression, traumatic stress, burnout and secondary trauma, and reviewing the individual’s lifestyle and coping skills. In addition, supervisors and managers have a duty to monitor the behaviour of all their workers, keeping an eye out for any changes that may suggest that someone needs extra help.
Trauma counselling
Trauma counselling provides support to help people who are experiencing symptoms of traumatic stress. Where traumatic stress is recognised early, trauma counselling should not require more than six sessions to deal with a number of responses including nightmares, distressing images, troubling thoughts and nervousness.
There are a number of trauma counselling approaches that can be used to support workers who are having difficulties; however, it is important that the therapist is experienced in working in a business environment. The models of counselling that have been found to be most effective in dealing with trauma are trauma-focused cognitive behavioural therapy (CBT) and eye movement desensitisation and reprocessing (EMDR).
Review and evaluation
Organisations need to review their support programme regularly. Ideally, there should be a named individual responsible for undertaking the review and evaluation process. This person should then present a report on the levels of stress/personal growth, engagement with the process, any hotspots of stress, actions taken to reduce stress and the worker’s satisfaction with the process.
Creating a trauma-informed workplace
To struggle through a traumatic experience it leading to personal and organisational growth and development is a lost opportunity. Research that looked at the way people from different working backgrounds responded to traumatic exposures found that higher levels of personal discomfort were accompanied by more learning and personal development (Tehrani, 2012) – in other words, the more pain, the greater the gain. This gain could be predicted by looking at a number of personal and organisational factors; workers were more likely to increase their learning and development if they maintained a healthy work-life balance, practiced their spiritual beliefs, took regular exercise, had hobbies and ate a healthy diet. Equally important was the support that a team leader, manager and the organisation offered in providing time for the individual to reflect on the effect that the traumatic exposure had on them in formal individual or group supervision sessions facilitated by a trained peer or professional supervisor.
It should be remembered that organisations are living systems and therefore they are also vulnerable to becoming traumatised by the nature of the work undertaken. Public-service organisations including those involved with health, social services, education and policing are likely to demonstrate trauma symptoms in the way that they respond to their workers, users and other stakeholders. Traumatic exposure creates an organisational shadow side destructive to relationships and ultimately to the organisation itself. The box below provides some indication of the signs that indicate organisational traumatisation.
Box 2: Symptoms and signs of traumatised organisations |
|
| Symptom | Signs |
| Arousal | Reactive management style; extreme responses; bullying; reckless decision making; blaming; inability to concentrate on complex issues. |
| Avoidance | Silencing of alternative views; protection of the status quo; inability to accept organisational shortcomings; punishment of whistleblowers. |
| Re-experience | Repetition of failed strategies; extreme reaction to reminders of past failures; irrational responses to perceived threats. |
| Negative mood/beliefs | Feeling that no one can be trusted; blaming; organisational loss of purpose; isolation; loss of imagination and creativity; depression. |
Organisations have a vital role in helping workers deal with trauma by supporting the management of traumatic events and then creating individual and organisational meaning in order to maximise learning. To do this, businesses have to recognise their own burden of trauma and engage more deeply in improving a firm’s emotional strengths and vitality. This organisational growth is facilitated by engaging in open communication with workers and stakeholders and developing a culture that encourages the possibility of social learning, emotional resilience and growth.
References
Tehrani N (2011). Managing Trauma in the Workplace: Supporting Workers and Organisations. Hove; Routledge.
Sign up to our weekly round-up of HR news and guidance
Receive the Personnel Today Direct e-newsletter every Wednesday
Tehrani N (2010). “Compassion fatigue: experiences in occupational health, human resources, counselling and police”. Occupational Medicine; vol.60, issue 2, pp.133-138.
